 Microorganisms A microorganism (from the mikros, "small" and , organismós, "organism"") is a microscopic living organism, which may be single-celled or multicellular. The study of microorganisms is called microbiology, a subject that began with the discovery of microorganisms in 1674 by Antonie van Leeuwenhoek, using a microscope of his design. Microorganisms are very diverse and include all the bacteria and archaea and almost all the protozoa. They also include some fungi, algae, and certain animals, such as rotifers. Many macroscopic animals and plants have microscopic juvenile stages. Some microbiologists also classify viruses (and viroids) as microorganisms, but others consider these as nonliving. Microorganisms live in every part of the biosphere, including soil, hot springs, "seven miles deep" in the ocean, "40 miles high" in the atmosphere and inside rocks far down within the Earth's crust (see also endolith). Microorganisms, under certain test conditions, have been observed to thrive in the vacuum of outer space. The total amount of soil and subsurface bacterial carbon is estimated as 5 x 1017 g, or the "weight of the United Kingdom". The mass of prokaryote microorganisms — which includes bacteria and archaea, but not the nucleated eukaryote microorganisms — may be as much as 0.8 trillion tons of carbon (of the total biosphere mass of 4 trillion tons). Read original post here: https://local.google.com/place?id=9845698472642226705&use=posts&lpsid=CIHM0ogKEICAgICj47zJVA
0 Comments
 Here's a comprehensive checklist, that outlines the essential steps and examinations involved before the implant process can commence: Thorough Preoperative Examinations: Blood Test: Assessing overall health and identifying any underlying conditions that may affect the success of the implants. By diligently following the golden list and adhering to preoperative examinations and preparations, patients can set the stage for successful dental implant placement. With proper care and attention, dental implants can offer a lasting solution for restoring oral health and confidence. Check out our previous post: Read original post here: https://local.google.com/place?id=9845698472642226705&use=posts&lpsid=CIHM0ogKEICAgICjqYOobA  Fluoride Mouthwashes, Fluoride Dentifrices, And Other Uses Of Fluorides In Control Of Caries This medication is applied to teeth to prevent cavities. Fluoride is a mineral that works by making the teeth stronger and more resistant to decay caused by acid and bacteria. Do not use this medication in children younger than 6 years unless directed to do so by your dentist/doctor. How to use Fluoride Mouthwash Solution Carefully watch children during use and teach proper rinsing habits to avoid swallowing. To get the most benefit, you should not eat, drink, or rinse your mouth for at least 30 minutes after using the solution. Dosage is based on age and the amount of fluoride in your drinking water. Do not exceed the recommended dose without checking with your dentist/doctor. Doing so will not do more to prevent cavities but may lead to side effects instead. Use this medication regularly to get the most benefit from it. To help you remember, use it at the same time each day. Do not treat this medication like a normal mouthwash: do not use it more often than prescribed, or just to freshen your breath. Read original post here: https://local.google.com/place?id=9845698472642226705&use=posts&lpsid=CIHM0ogKEICAgICjtp2syQE  Now that your implants have seamlessly integrated with your jawbone, it's crucial to prioritize proper care to maintain their longevity and functionality. Here's a brief guide on how to care for your dental implant-supported teeth: Routine Dental Hygiene: Treat your implants like natural teeth by adhering to a regular oral hygiene routine. Brush at least twice daily. Don't forget to floss between your implants and natural teeth to remove plaque and debris. Biannual Dental Visits: Schedule check-ups with your dentist every six months. These routine visits allow your dentist to assess the health of your implants, gums, and surrounding teeth. While adjustments or tightening may occasionally be necessary, it's not a frequent occurrence. Mindful Eating Habits: Enjoy your favorite foods with confidence, knowing that your dental implants can withstand normal chewing forces. However, it's wise to avoid very hard or sticky foods that may exert excessive pressure on your implants and surrounding structures. By incorporating these simple yet essential practices into your daily routine, you'll ensure the longevity and success of your dental implant-supported teeth. With proper care and regular dental check-ups, you can continue to smile, eat, and live confidently for years to come. Check out our previous post: Read original post here: https://local.google.com/place?id=9845698472642226705&use=posts&lpsid=CIHM0ogKEICAgICjopL-Yg  Dentures, also known as false teeth, are prosthetic devices constructed to replace missing teeth; they are supported by the surrounding soft and hard tissues of the oral cavity. Conventional dentures are removable (removable partial denture or complete denture). However, there are many different denture designs, some of which rely on bonding or clasping onto teeth or dental implants (fixed prosthodontics). There are two main categories of dentures, the distinction being whether they are used to replace missing teeth on the mandibular arch or the maxillary arch. Read original post here: https://local.google.com/place?id=9845698472642226705&use=posts&lpsid=CIHM0ogKEICAgICjqInKnAE  The first thing you can expect after getting your implants is an improved smile immediately after the procedure. Enjoy it, but a little care must be taken for best results. Before getting up and driving home, wait for the anesthesia to wear out completely. You can use cold packs or press on dry gauze pads to stop it. Avoid hot drinks for a while, and do not eat until anesthesia has worn off completely. In the next two days avoid strenuous movements. A little bit of swelling is also normal and will at its peak in about two days. A little bit of warmth applied to the cheeks will help reduce it. Slight pain is quite normal after surgery. Keep the mouth as clean as possible. Continue using the mouth wash for at least a weak, and every time try to hold the liquid over the site of surgery for some time. Mouth rinses with warm saline water will also aid quick relief from swelling and pain. Resume your daily brushing, but avoid the surgery sites until properly cured. While eating avoid the sites of surgery, and rinse after food. Avoid smoking until the wounds heal. After the wound has healed, and in about three to six months your implant will have firmly integrated with the bone around it. Now your teeth are like natural teeth. Enjoy life while maintaining routine dental hygiene and six-monthly visits for inspection. Check out our previous post: Read original post here: https://local.google.com/place?id=9845698472642226705&use=posts&lpsid=CIHM0ogKEICAgIDDl9jf8wE  A dental prosthesis is an intraoral (inside the mouth) prosthesis used to restore (reconstruct) intraoral defects such as missing teeth, missing parts of teeth, and missing soft or hard structures of the jaw and palate. Prosthodontics is the dental specialty that focuses on dental prostheses. Such prostheses are used to rehabilitate mastication (chewing), improve aesthetics, and aid speech. A dental prosthesis may be held in place by connecting to teeth or dental implants, by suction, or by being held passively by surrounding muscles. Like other types of prostheses, they can either be fixed permanently or removable; fixed prosthodontics and removable dentures are made in many variations. Permanently fixed dental prostheses use dental adhesive or screws, to attach to teeth or dental implants. Removal prostheses may use friction against parallel hard surfaces and undercuts of adjacent teeth or dental implants, suction using the mucous retention (without or without aid from denture adhesives), and by exploiting the surrounding muscles and anatomical contours of the jaw to passively hold in place. Some examples of dental prostheses include: dentures, partial denture, palatal obturator, orthodontic appliance, dental implant, crown, bridge. Read original post here: https://local.google.com/place?id=9845698472642226705&use=posts&lpsid=CIHM0ogKEICAgIDD7dCroAE A dental hygienist is a licensed dental professional who is registered with a dental association or regulatory body within their country of practice. They are a primary healthcare professional who works independent of, or alongside dentists and other dental professionals in a team to provide full oral health care. They have the training and education that focus and specialise in the prevention and treatment of oral disease. They can choose to work in a range of dental settings from independent practice, private practice, specialists practices to public sector; and can also work in residential aged care facilities. 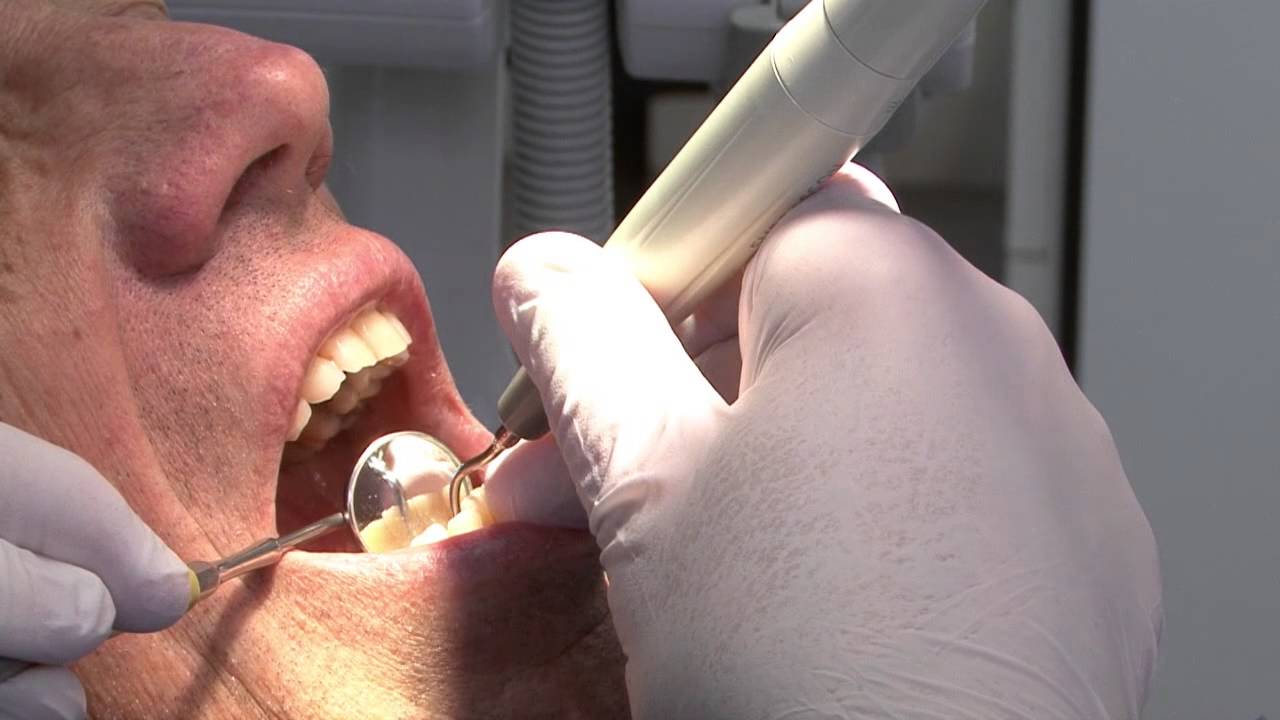
Dental hygienists have a specific scope of clinical procedures they provide to their patients. They assess a patients condition in order to offer patient-specific preventative and educational services to promote and maintain good oral health. The use of therapeutic methods assists their patients in controlling oral disease, while providing tailored treatment plans that emphasize the importance of behavioral changes . In most jurisdictions, hygienists work for a dentist or dental specialist, and some are licensed to administer local anesthesia and perform dental radiography. The major role of a dental hygienist is to perform periodontal therapy which includes things such periodontal charting, periodontal debridement (scaling and root planing), prophylaxis (cleaning) for patients with periodontal disease. In addition dental hygienists are able to perform examinations, make diagnosis, take intraoral radiographs, dental sealants, administer fluoride, and provide patient specific oral hygiene instruction. They are also able to work at an orthodontic clinic and can perform many tasks there. Such as selecting and sizing of orthodontic bands for dental braces, the removal of orthodontic appliances and are able to make dental impressions for the construction of study casts and mouthguards. Dental hygienists work together with other dental professionals, with a higher number working at general practices with dentists, dental therapists and oral health therapists. A smaller number work at specialist practices alongside orthodontists and periodontists. They help with the contribution of an interdisciplinary approach, aiming to provide optimum oral health care to their patients. Dental hygienists also aim to work interprofessionally to provide holistic oral health care in the best interest of their patient. Dental hygienists also offer expertise in their field and can provide a dental hygiene diagnosis, which is an integral component of the comprehensive dental diagnosis. Other areas that relate to dentistry that dental hygienists can be involved in are: • Research: They can carry out clinical studies and trials alongside specialists in teaching institutions. • Professional Education: They are able to provide education by teaching and training dental hygiene students and dental assistants. They can also choose to present research at a variety of different events and seminars within their industry. • Community health: They provide assistance and group talks in community dental clinics, residential care, hospitals and nursing homes. Read original post here: https://forestray.dentist/kb/dental-hygienists/ A bridge is a fixed dental restoration (a fixed dental prosthesis) used to replace one or more missing teeth by joining an artificial tooth definitively to adjacent teeth or dental implants. 
DefinitionsFixed bridge: A dental prosthesis that is definitively attached to natural teeth and replaces missing teeth. Abutment: The tooth that supports and retains a dental prosthesis. Pontic: The artificial tooth that replaces a missing natural tooth. Retainer: The component attached to the abutment for retention of the prosthesis. Retainers can be major or minor. Unit: Pontics and abutment teeth are referred to as units. The total number of units in a bridge is equal to the number of pontics plus the number of abutment teeth. Saddle: The area on the alveolar ridge which is edentulous where at least one missing tooth is to be reinstated. Connector: Joins the pontic to the retainer or two retainers together. Connectors may be fixed or movable. Span: The length of the alveolar ridge between the natural teeth where the bridge will be placed. Resin bonded bridge: A dental prostheses where the pontic is connected to the surface of natural teeth which are either unprepared or minimally prepared. Read original post here: https://forestray.dentist/kb/dental-bridge/ The alveolar process or alveolar bone is the thickened ridge of bone that contains the tooth sockets on the jaw bones (in humans, the maxilla and the mandible). The structures are covered by gums as part of the oral cavity. The synonymous terms alveolar ridge and alveolar margin are also sometimes used more specifically to refer to the ridges on the inside of the mouth which can be felt with the tongue, either on roof of the mouth between the upper teeth and the hard palate or on the bottom of the mouth behind the lower teeth. 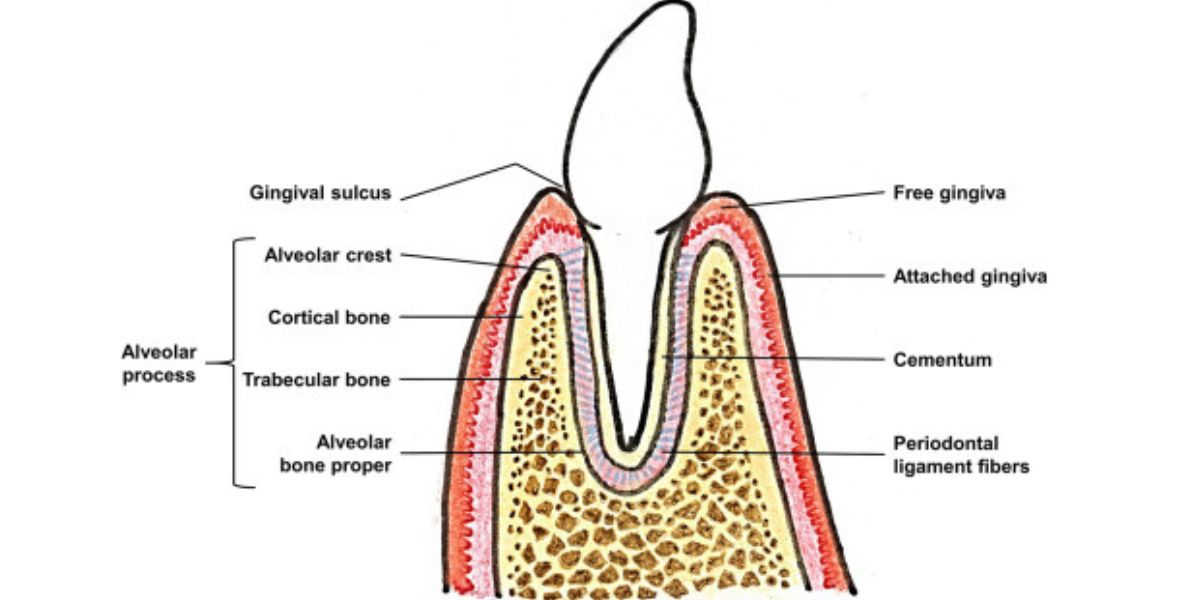 Read original post here: https://forestray.dentist/kb/alveolar-ridge/ Orthodontic retainers are custom-made devices, usually made of wires or clear plastic, that hold teeth in position after surgery or any method of realigning teeth. They are most often used before or after dental braces to keep teeth in position while assisting the adjustment of the surrounding gums to changes in the bone. Most patients are required to wear their retainer(s) every night at first, with many also being directed to wear them during the day – at least initially. There are four types of retainers typically prescribed by orthodontists and dentists: Hawley, Essix, Zendura, and Bonded (Fixed) retainers. 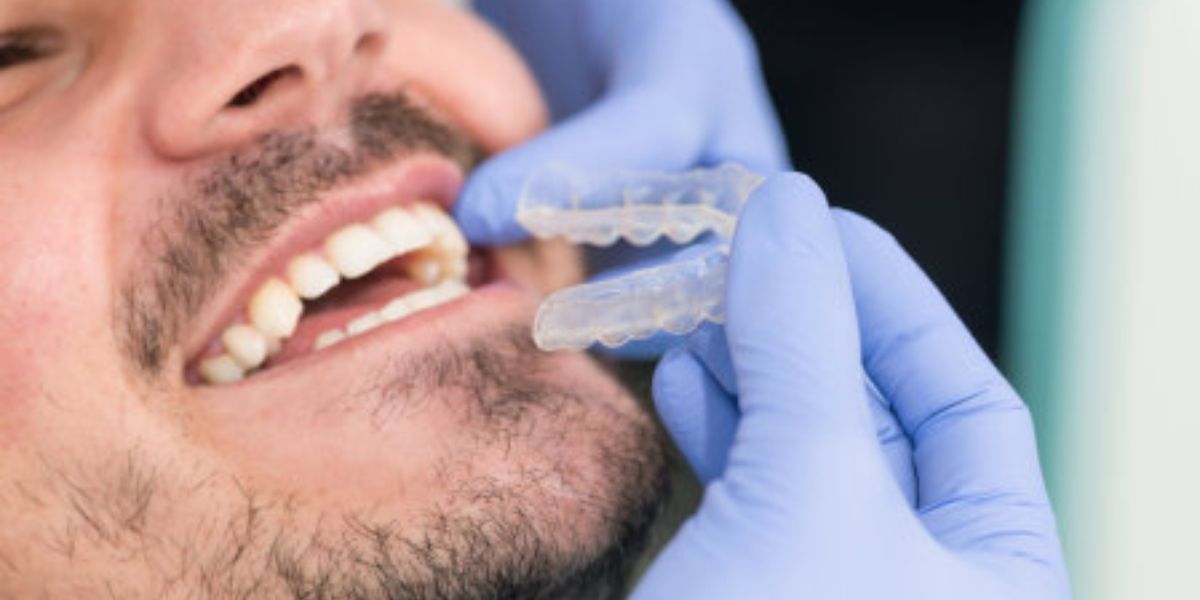 Read original post here: https://forestray.dentist/kb/retainer/ In orthodontics, a malocclusion is a misalignment or incorrect relation between the teeth of the upper and lower dental arches when they approach each other as the jaws close. The English-language term dates from 1864;Edward Angle (1855-1930), the "father of modern orthodontics", popularised it. The word "malocclusion" derives from occlusion, and refers to the manner in which opposing teeth meet (mal- + occlusion = "incorrect closure"). 
The malocclusion classification is based on the relationship of the mesiobuccal cusp of the maxillary first molar and the buccal groove of the mandibular first molar. If this molar relationship exists, then the teeth can align into normal occlusion. According to Angle, malocclusion is any deviation of the occlusion from the ideal. However, assessment for malocclusion should also take into account aesthetics and the impact on functionality. If these aspects are acceptable to the patient despite meeting the formal definition of malocclusion, then treatment may not be necessary. It is estimated that nearly 30% of the population have malocclusions that are categorised as severe and definitely benefit from orthodontic treatment. Read original post here: https://forestray.dentist/kb/malocclusion/ Dentifrices are agents used along with a toothbrush to clean and polish natural teeth. They are supplied in paste, powder, gel or liquid form. There have been many dentifrices produced over the years, many focusing on marketing strategies to sell products, such as offering whitening capabilities. The most essential dentifrice recommended by dentists is toothpaste which is used in conjunction with a toothbrush to help remove food debris and dental plaque. Dentifrice is also the French word for toothpaste. 
ToothpasteToothpaste is a dentifrice used in conjunction with a toothbrush to help maintain oral hygiene. The essential components are an abrasive, binder, surfactant and humectant. Other ingredients are also used. The main purpose of the paste is to help remove debris and plaque with some marketed to serve accessory functions such as breath freshening and teeth whitening. Tooth powderThe use of powdered substances such as charcoal, brick, and salt for cleaning teeth has been historically widespread in India, particularly in rural areas. In modern times, baking soda has been the most commonly used tooth powder. It has been positioned as a cost-effective substitute for toothpaste, as it can be applied with the index finger without requiring use of a toothbrush. MouthwashMouthwash may come in a variety of compositions, claiming to kill bacteria that make up plaque or to freshen breath. In their basic form, they are usually recommended for use after brushing but some manufacturers recommend pre-brush rinsing. Read original post here: https://forestray.dentist/kb/dentifrice/ Sodium bicarbonate comes from an outdated naming system and is based on the observation that there is two times as much carbonate (CO3) in sodium bicarbonate (NaHCO3) and other bicarbonates as in sodium carbonate (Na2CO3) and other carbonates. (IUPAC name: sodium hydrogen carbonate) is the chemical compound with the formula NaHCO3. Sodium bicarbonate is a white solid that is crystalline but often appears as a fine powder. It has a slightly salty, alkaline taste resembling that of washing soda (sodium carbonate). 
The natural mineral form is nahcolite. It is a component of the mineral natron and is found dissolved in many mineral springs. Since it has long been known and is widely used, the salt has many related names such as baking soda, cooking soda, and bicarbonate of soda. It is among the food additives encoded by European Union, identified by the initials E 500. It is also used as an ingredient in some mouthwashes. It has anti-caries and abrasive properties. It works as a mechanical cleanser on the teeth and gums, neutralizes the production of acid in the mouth, and also acts as an antiseptic to help prevent infections. Read original post here: https://forestray.dentist/kb/baking-soda/ Canary Wharf is a major business district located in Tower Hamlets, London. It is one of the United Kingdom's two main financial centres – along with the traditional City of London – and contains many of the UK's tallest buildings, including the second-tallest, One Canada Square. 
Canary Wharf contains around of office and retail space, of which around is owned by Canary Wharf Group. Around 105,000 people work in Canary Wharf and it is home to the world or European headquarters of numerous major banks, professional services firms and media organisations including Barclays, Citigroup, Clifford Chance, Credit Suisse, Infosys, Fitch Ratings, HSBC, J.P. Morgan, KPMG, MetLife, Moody's, Morgan Stanley, RBC, Skadden, State Street and Thomson Reuters. It is located in the West India Docks on the Isle of Dogs in the Borough of Tower Hamlets in East London. The West India Docks once formed part of the busiest port in the world. After the docks were closed in 1980 the British Government adopted various policies to stimulate the redevelopment of the area, including through the creation of the London Docklands Development Corporation in 1981 and granting the Isle of Dogs Enterprise Zone status in 1982. In 1987 the Canadian company Olympia and York agreed to construct a major office development on the Isle of Dogs, with construction commencing in 1988. Read original post here: https://forestray.dentist/kb/canary-wharf/ Buckingham Palace is the London residence and principal workplace of the monarchy of the United Kingdom. Located in the City of Westminster, the palace is often at the centre of state occasions and royal hospitality. It has been a focus for the British people at times of national rejoicing. 
Originally known as Buckingham House, the building which forms the core of today's palace was a large townhouse built for the Duke of Buckingham in 1703 on a site which had been in private ownership for at least 150 years. It was subsequently acquired by King George III in 1761 as a private residence for Queen Charlotte and was known as "The Queen's House". During the 19th century it was enlarged, principally by architects John Nash and Edward Blore, who formed three wings around a central courtyard. Buckingham Palace finally became the official royal palace of the British monarch on the accession of Queen Victoria in 1837. The last major structural additions were made in the late 19th and early 20th centuries, including the East front, which contains the well-known balcony on which the royal family traditionally congregates to greet crowds outside. However, the palace chapel was destroyed by a German bomb during World War II; the Queen's Gallery was built on the site and opened to the public in 1962 to exhibit works of art from the Royal Collection. The original early 19th-century interior designs, many of which still survive, included widespread use of brightly coloured scagliola and blue and pink lapis, on the advice of Sir Charles Long. King Edward VII oversaw a partial redecoration in a Belle Époque cream and gold colour scheme. Many smaller reception rooms are furnished in the Chinese regency style with furniture and fittings brought from the Royal Pavilion at Brighton and from Carlton House. The Buckingham Palace Garden is the largest private garden in London. The state rooms, used for official and state entertaining, are open to the public each year for most of August and September, as part of the Palace's Summer Opening. Read original post here: https://forestray.dentist/kb/buckingham-palace/ The East End of London is an area of London, England, east of the Roman and medieval walled City of London and north of the River Thames. Although not defined by universally accepted formal boundaries, the River Lea can be considered another boundary. It is universally agreed, however, that the East End is to be distinguished from East London, which covers a much wider area. 
Use of the term East End in a negative connotations began in the late 19th century, as the expansion of the population of London led to extreme overcrowding throughout the area and a concentration of poor people and immigrants. The problems were exacerbated with the construction of St Katharine Docks (1827) and the central London railway termini (1840–1875) that caused the clearance of former slums and rookeries, with many of the displaced people moving into the East End. Over the course of a century, the East End became synonymous with poverty, overcrowding, disease and criminality. Originally it was an area characterised by villages clustered around the City walls or along the main roads, surrounded by farmland, with marshes and small communities by the River, serving the needs of shipping and the Royal Navy. The area attracted large numbers of rural people looking for employment. Successive waves of foreign immigration began with Huguenot refugees. They were followed by Irish weavers, Ashkenazi Jews and, in the 20th century, Bangladeshis. Many of these immigrants worked in the clothing industry. This brought the attentions of social reformers and led to the formation of workers unions at the end of the century. The Second World War devastated much of the East End, with its docks, railways and industry forming a continual target for bombing leading to dispersal of the population to new suburbs being built in the 1950s. The closure of the last of the East End docks in the Port of London in 1980 created further challenges and led to attempts at regeneration and the formation of the London Docklands Development Corporation. The Canary Wharf development, improved infrastructure, and the Olympic Park mean that the East End is undergoing further change. Read original post here: https://forestray.dentist/kb/east-end/ Health care (or healthcare) is the diagnosis, treatment, and prevention of disease, illness, injury, and other physical and mental impairments in human beings. Health care is delivered by practitioners in allied health, dentistry, midwifery (obstetrics), medicine, nursing, optometry, pharmacy, psychology and other health professions. It refers to the work done in providing primary care, secondary care, and tertiary care, as well as in public health. Access to health care varies across countries, groups, and individuals, largely influenced by social and economic conditions as well as the health policies in place. Countries and jurisdictions have different policies and plans in relation to the personal and population-based health care goals within their societies. 
Health care systems are organizations established to meet the health needs of target populations. Their exact configuration varies between national and subnational entities. In some countries and jurisdictions, health care planning is distributed among market participants, whereas in others, planning occurs more centrally among governments or other coordinating bodies. In all cases, according to the World Health Organization (WHO), a well-functioning health care system requires a robust financing mechanism; a well-trained and adequately-paid workforce; reliable information on which to base decisions and policies; and well maintained health facilities and logistics to deliver quality medicines and technologies. Health care can contribute to a significant part of a country's economy. In 2011, the health care industry consumed an average of 9.3 percent of the GDP or US$ 3,322 (PPP-adjusted) per capita across the 34 members of OECD countries. The USA (17.7%, or US$ PPP 8,508), the Netherlands (11.9%, 5,099), France (11.6%, 4,118), Germany (11.3%, 4,495), Canada (11.2%, 5669), and Switzerland (11%, 5,634) were the top spenders, however life expectancy in total population at birth was highest in Switzerland (82.8 years), Japan and Italy (82.7), Spain and Iceland (82.4), France (82.2) and Australia (82.0), while OECD's average exceeds 80 years for the first time ever in 2011: 80.1 years, a gain of 10 years since 1970. The USA (78.7 years) ranges only on place 26 among the 34 OECD member countries, but has the highest costs by far. All OECD countries have achieved universal (or almost universal) health coverage, except Mexico and the USA. (see also international comparisons.) Health care is conventionally regarded as an important determinant in promoting the general physical and mental health and well-being of people around the world. An example of this was the worldwide eradication of smallpox in 1980, declared by the WHO as the first disease in human history to be completely eliminated by deliberate health care interventions. Read original post here: https://forestray.dentist/kb/health-services/ Preventative dentistry is a proactive approach to maintaining oral health, aimed at preventing dental issues like cavities and gum disease. It involves a partnership between dental professionals and patients, focusing on regular dental check-ups, professional cleanings, and educating patients on effective oral hygiene practices. Key components include teaching proper brushing and flossing techniques, recommending specific oral care products, and advising on healthy dietary choices. 
This approach is beneficial for individuals across all age groups. For children, it ensures the proper development of their teeth and instills good dental habits early on. Adults and seniors benefit from preventative dentistry by maintaining their natural teeth and avoiding the complications associated with dental diseases. Regular dental visits enable early detection and management of potential oral health issues, reducing the need for more complex and costly treatments in the future. Preventative dentistry also underscores the importance of daily personal care routines, such as brushing with fluoride toothpaste, flossing, and using mouthwash to remove food particles and plaque. Avoiding acidic and hard foods that can damage tooth enamel is another aspect of preventing dental erosion. For individuals engaged in sports or those who grind their teeth, using mouth guards is recommended to protect teeth from injury and wear. Overall, preventative dentistry is not just about avoiding dental problems; it's about promoting a lifetime of healthy smiles. By integrating professional dental services with good at-home oral care, individuals can significantly reduce their risk of dental diseases, contributing to their overall health and well-being. This holistic approach to dental care emphasizes the critical role of oral health in influencing a person's quality of life and general health. EAPD Guildeline on Early Childhood CariesRead original post here: https://forestray.dentist/kb/prevention/ Diagnosis is the identification of the nature and cause of a certain phenomenon. Diagnosis is used in many different disciplines with variations in the use of logics, analytics, and experience to determine "cause and effect". In systems engineering and computer science, it is typically used to determine the causes of symptoms, mitigations, and solutions.  Read original post here: https://forestray.dentist/kb/diagnosis/ Pathogenic bacteria are bacteria that can cause infection. This article deals with human pathogenic bacteria. Although most bacteria are harmless or often beneficial, several are pathogenic. One of the bacterial diseases with the highest disease burden is tuberculosis, caused by the bacterium Mycobacterium tuberculosis, which kills about 2 million people a year, mostly in sub-Saharan Africa. Pathogenic bacteria contribute to other globally important diseases, such as pneumonia, which can be caused by bacteria such as Streptococcus and Pseudomonas, and foodborne illnesses, which can be caused by bacteria such as Shigella, Campylobacter, and Salmonella. Pathogenic bacteria also cause infections such as tetanus, typhoid fever, diphtheria, syphilis, and leprosy. Koch's postulates are criteria designed to establish a causal relationship between a causative microbe and a disease. 
Dental infections originate in the tooth or its supporting structures and can spread to the surrounding tissues. When facial structures are compromised the infection tends to originate from necrotic pulp, periodontal pockets, or pericoronitis. Dental infections have always been common and were one of the leading causes of death hundreds of years ago. The London England Bills of mortality in the 1600s reported teeth infections as the 5th or 6th leading cause of death. In 1908 it was believed that dental infections were associated with a mortality of 10 to 40% . Fortunately, due to improved dental hygiene, modern dentistry, and antibiotics, dental infections are rarely life-threatening today. EtiologyDental infections most commonly occur when bacteria invade the pulp and spread to surrounding tissues; this can be due to dental caries, trauma, or dental procedures. Periodontal infections caused by periodontal pathogens first involve the gingival tissues causing gingivitis and, over time, periodontitis. The periodontal disease mostly results from poor or ineffective dental hygiene leading to plaque and calculus accumulation and subsequent inflammation of tissues that support the teeth, alveolar bone, periodontal ligament, and cementum. The etiology of periodontitis is multifactorial; while bacteria initiate them, the clinical presentation and outcome of the different forms of the disease are in the end determined by the inflammatory response and modifying and predisposing factors. The disease progression seems to be regulated by environmental and genetic factors specific in each patient. Streptococcus mutans is considered as the primary etiologic agent of dental caries, an infectious disease. This pathogen can access the bloodstream during dental procedures, causing opportunistic systemic infections. Thus, bacteremia, through the adhesion to the endocardium, is involved in infective endocarditis and peripheral arterial disease. EpidemiologyIt is estimated that 13% of adults seek dental care for dental infection or toothache within four years and that 1 per 2600 head of the population in the United States is hospitalized due to dental infections. More than 1 in 5 people have untreated dental caries, and 3 in 4 people had at least one dental restoration during their life. Periodontitis is also common, with estimations that 35% of all Americans age 30 to 90 are afflicted. More than 1 in 5 people have untreated dental caries, and 3 in 4 people had at least one dental restoration during their life. Periodontal disease is also common, with estimations that 35% of Americans age 30 to 90 are afflicted. Furthermore, the prevalence of dental caries varies significantly by socioeconomic factors. Untreated dental caries were more than 2.5 times as common in those living 100% below the poverty level (41.9%) relative to those living 200% above the federal poverty level or higher (16.6%). The prevalence of dental caries is also dynamic during the patients' lifetime. Dental caries are present in 90% of adults and 42% of children ages 6 to 19 years. Dental caries did not appear to vary much with age except that adolescents age 12 to 19 were found to have a lower rate of untreated dental caries even when compared to children ages 5 to 11. Read original post here: https://forestray.dentist/kb/bacterial-infection/ Dental fear (also called dental phobia, odontophobia, dentophobia, dentist phobia, and dental anxiety) is the fear of dentistry and of receiving dental care. However, it has been suggested that use of the term dental phobia should not be used for people who do not feel that their fears are excessive or unreasonable, and instead resemble individuals with post-traumatic stress disorder, caused by previous traumatic dental experiences.  Read original post here: https://forestray.dentist/kb/dental-phobia/ Alveolar osteitis is inflammation of the alveolar bone (i.e., the alveolar process of the maxilla or mandible). Classically, this occurs as a postoperative complication of tooth extraction. Alveolar osteitis usually occurs where the blood clot fails to form or is lost from the socket (i.e., the defect left in the gum when a tooth is taken out). This leaves an empty socket where bone is exposed to the oral cavity, causing a localized alveolar osteitis limited to the lamina dura (i.e., the bone which lines the socket). This specific type of alveolar osteitis is also known as dry socket or, less commonly, fibrinolytic alveolitis, and is associated with increased pain and delayed healing time. Dry socket occurs in about 0.5–5% of routine dental extractions, and in about 25–30% of extractions of impacted mandibular third molars (wisdom teeth which are buried in the bone). 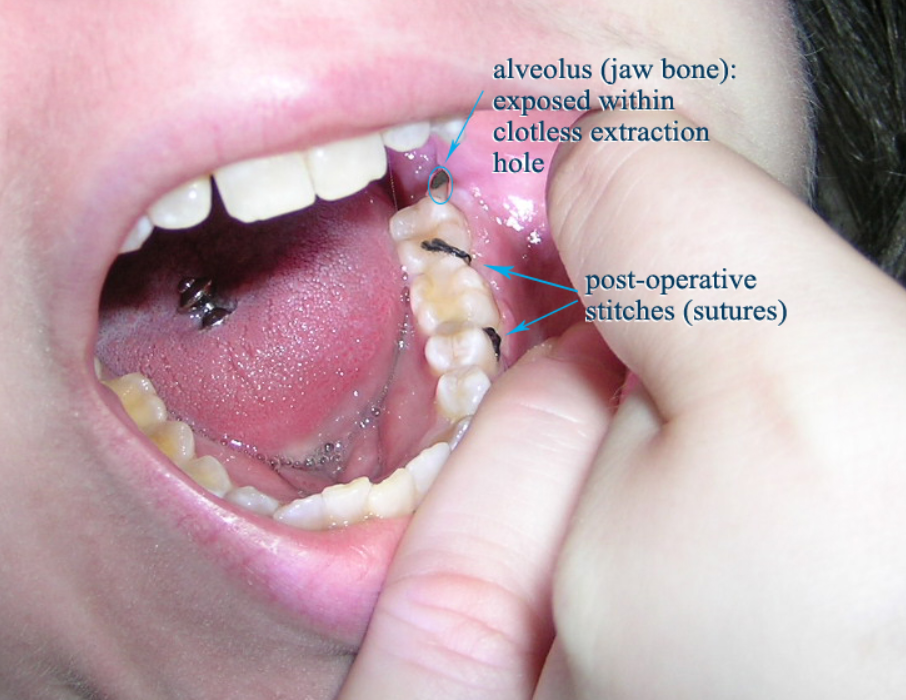 Read original post here: https://forestray.dentist/kb/alveolar-osteitis/ In the United States, Canada, and Australia, there are nine recognized dental specialties in which some dentists choose to train and practice, in addition to or instead of general dentistry. To become a specialist requires training in a residency or advanced graduate training program. Once a residency is completed, the doctor is granted a certificate of specialty training. 
Many specialty programs have optional or required advanced degrees such as a master's degree, such as the Master of Science (MS or MSc), Master of Dental Surgery/Science (MDS/MDSc), Master of Dentistry (MDent), Master of Clinical Dentistry (MClinDent), Master of Philosophy (MPhil), Master of Medical Science (MMS or (MMSc); doctorate such as Doctor of Clinical Dentistry (DClinDent), Doctor of Medical Science/Sciences (DMSc), or PhD;or medical degree: Doctor of Medicine/Bachelor of Medicine, Bachelor of Surgery (MD/MBBS) specific to maxillofacial surgery and sometimes oral medicine). Read original post here: https://forestray.dentist/kb/dental-specialties/ Occlusal trauma is a dental term that refers to the damage incurred when teeth are left in traumatic occlusion without proper treatment. When the maxillary and mandibular dental arches approach each together, as they do, for example, during chewing or at rest, the relationship between the opposing teeth is referred to as occlusion. If this occlusal relationship is not balanced properly it may result in pain, tenderness and even mobility of the affected teeth. 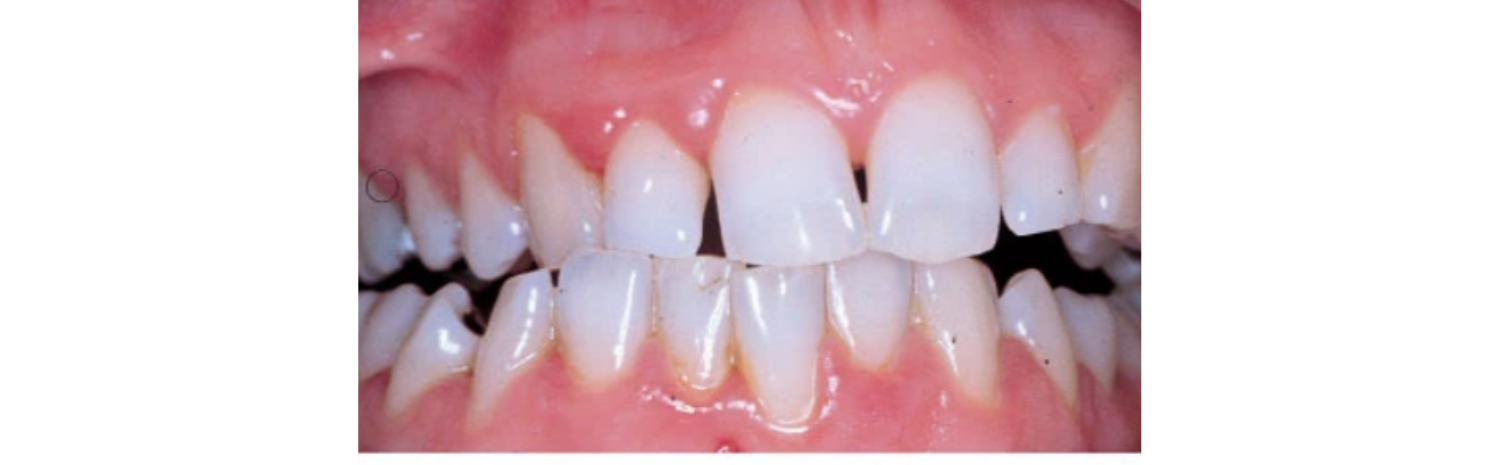
When the natural course of trauma, disease and dental treatment alters an individual's occlusion by removing or changing the occlusal (biting) surface of any of the teeth, that individual's teeth will come together, or occlude, differently, and their occlusion will change. When that change is detrimental to the manner in which the teeth occlude, the patient is said to possess a traumatic occlusion.traumatogenic occlusion - definition of traumatogenic occlusion in the Medical dictionary - by the Free Online Medical Dictionary, Thesaurus and Encyclopedia. Traumatic occlusion may cause a thickening of the cervical margin of the alveolar bone and widening of the periodontal ligament, although the latter is not pathognomonic for this condition. Read original post here: https://forestray.dentist/kb/occlusal-trauma/ |
|

 RSS Feed
RSS Feed
